Overview
Mitochondrial dysfunction is a condition that impacts the very powerhouses of our cells—mitochondria, which are crucial for energy production. When these organelles are impaired, it can lead to a range of health challenges, including metabolic disorders and neurodegenerative diseases. This issue affects millions of families, making it vital for us to understand its significance. We must continue to support ongoing research and advancements in diagnostic techniques to improve patient outcomes.
Imagine the challenges faced by families navigating this condition. The emotional toll can be overwhelming, and it’s essential to foster awareness and provide resources for those affected. By sharing knowledge and experiences, we can create a supportive community. Let’s work together to enhance understanding and offer hope to those in need. If you or someone you know is affected, consider reaching out for support and sharing your story. Together, we can make a difference.
Introduction
In the intricate world of cellular biology, mitochondria emerge as the powerhouses that fuel life itself. When these vital organelles falter, the consequences can be significant, leading to a cascade of health issues that touch the lives of millions. Mitochondrial dysfunction is not merely a medical anomaly; it is a pressing concern that intertwines with various diseases, ranging from metabolic disorders to neurodegenerative conditions. With over 50 million adults in the United States facing mitochondrial-related challenges, understanding the nuances of mitochondrial health is more critical than ever.
Recent advancements in research, including cutting-edge genomic techniques, are shedding light on the complexity of these disorders. This progress is paving the way for innovative diagnostic and treatment strategies that hold promise for those affected. As the medical community works diligently to unravel the mysteries of mitochondrial function, a comprehensive understanding of its implications becomes essential for improving patient outcomes and fostering effective advocacy. Together, we can navigate this intricate landscape and support one another in the journey toward better health.
Understanding Mitochondrial Dysfunction: Definition and Importance
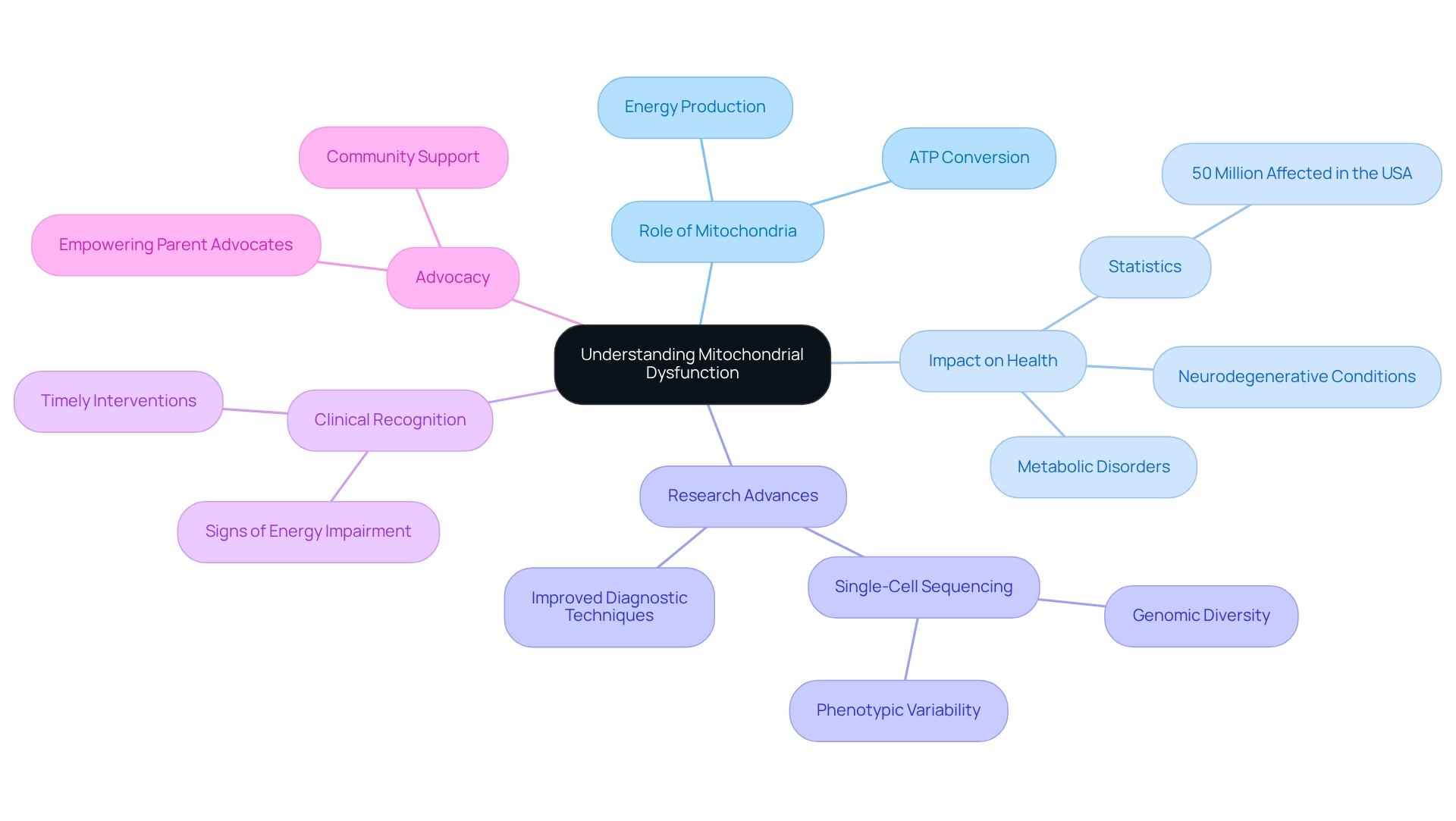
Understanding mitochondrial dysfunction begins with recognizing the vital role of mitochondria, the cellular organelles responsible for energy production. Often dubbed the 'powerhouses of the cell,' these structures convert nutrients into adenosine triphosphate (ATP), the essential energy currency that fuels our cellular activities. When the function of these cellular powerhouses is compromised, it can lead to various medical challenges, including metabolic disorders and neurodegenerative conditions.
The impact of mitochondrial dysfunction is significant, affecting over 50 million adults in the USA who face diseases linked to primary or secondary dysfunction. This statistic underscores the importance of understanding cellular function, especially as it relates to various diseases. Recent advancements in research, such as single-cell sequencing, have shed light on the genomic diversity and mutations that contribute to these cellular disorders.
For instance, a case study titled 'Single-Cell Sequencing in Mitochondrial Illness Research' demonstrates how this innovative method allows for the examination of individual cells, revealing insights into phenotypic variability and tissue-specific expressions of defects in these conditions.
Furthermore, enhanced diagnostic techniques have led to higher detection rates of mitochondrial disorders, highlighting the need for ongoing research and public awareness. Recent discoveries indicate that dedicated efforts have significantly improved our ability to identify cellular energy disorders across various regions. As we navigate the complexities of the human genome, advancements in sequencing technologies become essential for grasping the intricacies of cellular energy function.
In clinical settings, recognizing the signs of energy impairment can lead to timely interventions and better wellness outcomes. Understanding mitochondrial dysfunction is crucial, as the role of mitochondria in cellular processes is foundational to energy production and overall health. For parent advocates, grasping the nuances of cellular impairment is vital, as it can empower their advocacy efforts and enhance their ability to support children with related conditions.
Staying informed about the latest advancements in cell energy research is essential for both healthcare professionals and the public. We encourage you to share your experiences and insights, fostering a community of support and understanding.
Causes of Mitochondrial Dysfunction: Genetic and Environmental Factors
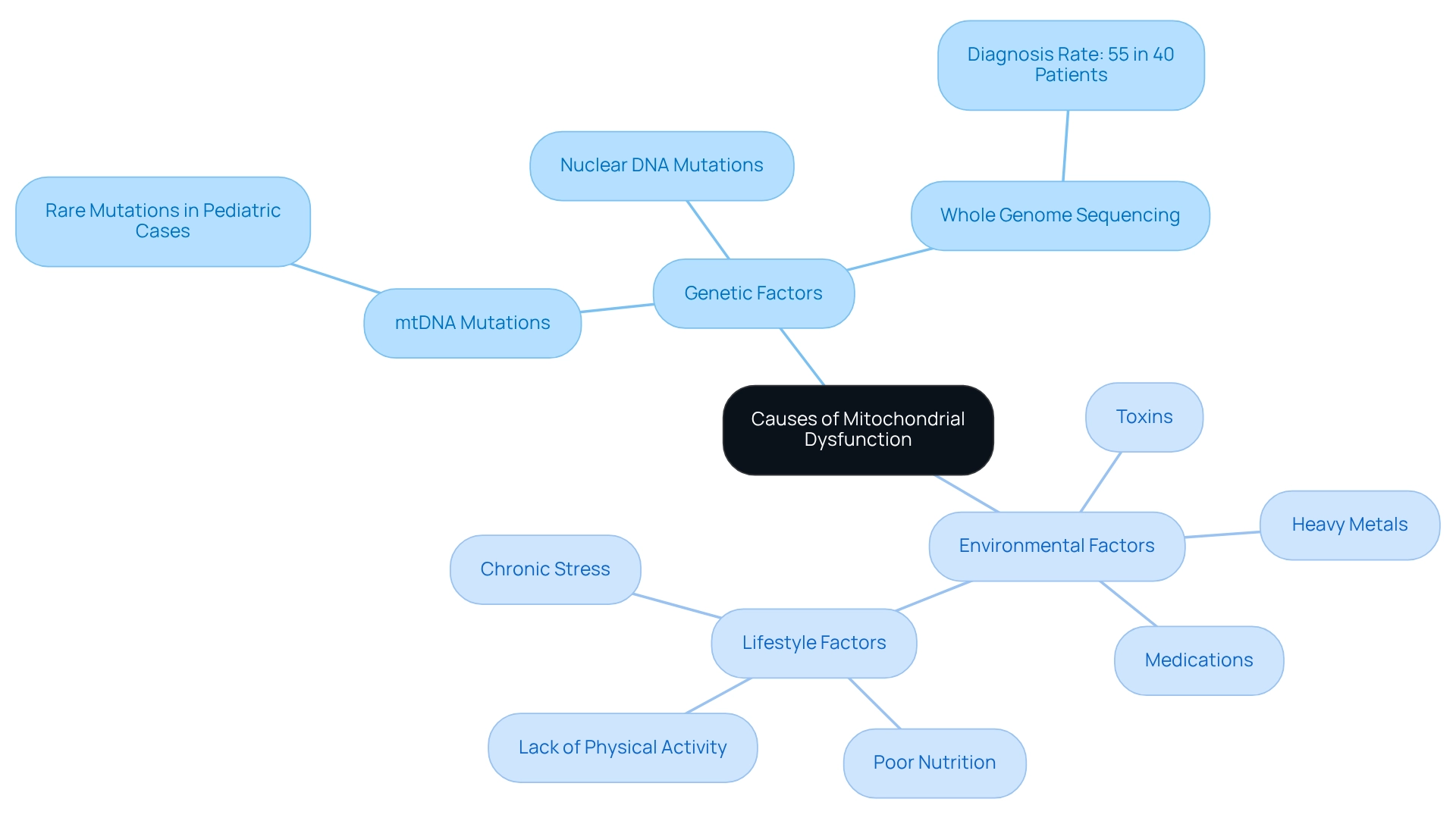
Mitochondrial dysfunction can arise from a complex interplay of genetic and environmental factors, which can be daunting to navigate. Genetic mutations, particularly those affecting mtDNA or nuclear DNA that encodes proteins associated with mitochondria, are significant contributors. These mutations may be inherited or occur spontaneously. Recent studies indicate that whole genome sequencing (WGS) has successfully identified 55% of patients within a specific group of 40 individuals facing cellular diseases. This underscores the importance of genetic testing in understanding these conditions and supporting affected families.
Environmental factors also play a crucial role in cellular health. Exposure to toxins, heavy metals, and certain medications can severely disrupt cellular energy production, creating additional challenges for families. For instance, studies have shown that rare mtDNA mutations are increasingly recognized as important factors in pediatric respiratory chain deficiencies. This challenges the earlier belief that such mutations were uncommon in children with energy-related disorders, highlighting the evolving understanding of these issues.
Moreover, lifestyle factors such as poor nutrition, lack of physical activity, and chronic stress can exacerbate cellular dysfunction. This emphasizes the need for a holistic approach to well-being, one that encompasses both physical and emotional health.
Experts emphasize the necessity of considering both genetic and environmental factors when evaluating mitochondrial dysfunction. A recent case study examined the implications of cellular variations in illness associations, revealing that the prevalence of certain mtDNA mutations in the general population could lead to misunderstandings about illness connections. This highlights the importance of careful interpretation of genetic data within clinical contexts, ensuring that families receive accurate information.
Furthermore, patient registries and collaborative networks are essential for advancing research on cellular energy disorders. They provide valuable insights into the complexities of these conditions, fostering a community of support.
As HP noted, collaboration and constructive feedback are vital in the writing process, emphasizing the importance of community in enhancing understanding in this field. Grasping the intricate reasons behind cellular energy failure is crucial for developing effective preventive measures and targeted treatments, ultimately empowering individuals to manage their health more effectively.
Recognizing the Symptoms: How Mitochondrial Dysfunction Manifests
Understanding mitochondrial dysfunction is essential. This condition can manifest through a variety of symptoms that significantly impact multiple organ systems, highlighting the vital role mitochondria play throughout the body. Common signs include fatigue, muscle weakness, and neurological disturbances, alongside metabolic irregularities. Many patients report challenges such as exercise intolerance, developmental delays, seizures, and gastrointestinal issues.
The variability of these symptoms can make diagnosis challenging, as they often overlap with other medical conditions. Recent findings reveal that approximately 80% of children with autism spectrum disorder (ASD) exhibit signs of cellular impairment, underscoring the urgent need for heightened awareness among healthcare professionals.
Recognizing these symptoms early is crucial for timely intervention, which can greatly improve the quality of life for those affected. Insights from neurologists emphasize the importance of a comprehensive approach to diagnosis, particularly in understanding mitochondrial dysfunction, as cellular issues can present differently across organ systems. Dr. Mark Tarnopolsky, a member of the advisory board, notes that "a comprehensive approach is crucial for the diagnosis and management of energy-related conditions," highlighting the need for collaboration among healthcare providers.
The phenomenon known as the genetic bottleneck can lead to significant variability in disease severity among siblings, reflecting the complex genetic factors at play. As research continues to evolve, it remains vital to understand the frequency and manifestations of cellular impairment. While statistics show that diagnosis rates are improving, many cases still go unrecognized.
By fostering a collaborative environment among parents, experts, and researchers, we can better address the challenges surrounding cellular energy issues and improve outcomes for those impacted. Together, we can make a difference.
Diagnosis of Mitochondrial Dysfunction: Methods and Challenges
Understanding mitochondrial dysfunction requires a thoughtful approach that includes clinical assessment, biochemical examinations, and genetic analysis. Healthcare providers typically start by gathering a comprehensive medical history and conducting a physical examination, followed by laboratory tests designed to evaluate metabolic function and cellular activity. Common diagnostic methods involve measuring lactate levels, performing muscle biopsies, and conducting genetic testing to pinpoint specific mutations associated with disorders of cellular energy production.
Yet, the diverse nature of cellular disorders presents significant challenges in diagnosis. For instance, only 43 (10%) of the genes linked to energy-producing organelle disorders are annotated in the Online Mendelian Inheritance in Man (OMIM) database as disorder genes with an associated phenotype and mode of inheritance. This complicates the identification of pathogenic variants. Furthermore, the lack of standardized definitions regarding pathogenicity and cellular positioning exacerbates the diagnostic challenges faced by healthcare professionals.
Case studies illustrate that the initial contact with healthcare providers can profoundly influence diagnostic outcomes. The survey titled "Role of Specialists in Mitochondrial Disease Diagnosis" examined how the first doctor seen by patients impacts the diagnostic process. It revealed that patients who first consulted specialists experienced notably fewer consultations before receiving a diagnosis compared to those who began with primary care physicians. While the overall time to diagnosis did not differ significantly, this underscores the critical need for improved access to specialists in energy metabolism disorders.
Expert insights emphasize the importance of understanding mitochondrial dysfunction, as the symptoms associated with cellular dysfunction can vary greatly among individuals. As J.LP. Thompson noted, "The data underlying the results presented in the study are available from J.LP. Thompson, (jlt12@cumc.columbia.edu)." As the landscape of cellular disorder diagnosis continues to evolve, ongoing education and collaboration among healthcare providers will be vital to enhance diagnostic accuracy and improve patient outcomes. Additionally, discrepancies in responses across registries and changes in disease management highlight the complexities involved in the diagnostic landscape, further emphasizing the need for standardized definitions in classifying mitochondrial-related disease genes.
Treatment Approaches for Mitochondrial Dysfunction: Current Strategies and Innovations
Caring for cellular energy dysfunction is primarily supportive, tailored to meet the unique symptoms and needs of each individual. Current strategies encompass dietary changes and nutritional supplements, such as coenzyme Q10 and L-carnitine, which have been shown to effectively support cellular function. Additionally, exercise programs play a vital role; recent studies indicate that customized exercise training can significantly enhance quality of life and metabolic function for those with primary cellular energy disorders.
As Dr. Andrea Gropman insightfully notes, "Current treatments are largely supportive, aimed at avoidance or mitigation of metabolic decompensation and treatment of specific organ-system dysfunction." Exciting new treatments, including gene therapy and pharmacological agents targeting cellular pathways, are currently under investigation, showing promising results in clinical trials. A recent review highlighted the evolving landscape of treatments for PMD, emphasizing the potential of novel therapies, dietary supplementation, and exercise training to become mainstream options in the near future.
Notably, NIR-LED therapy has been assessed in an open-label phase 1/2 clinical trial involving four patients with LHON, showcasing the ongoing research in this area.
A multidisciplinary approach is essential for optimizing care and improving patient outcomes. Collaboration among dietitians, physical therapists, and medical specialists ensures that treatment plans are comprehensive and effective. Insights from nutritionists suggest that specific dietary modifications can play a crucial role in enhancing cellular health, with real-world examples demonstrating the positive impact of such changes on patient well-being.
Recent advancements in understanding the genetics and pathophysiology of PMD have paved the way for new pharmacological and non-pharmacological therapies, many of which are currently in clinical trials. As we progress in this field, addressing mitochondrial issues will necessitate a deeper understanding of mitochondrial dysfunction, alongside the incorporation of cutting-edge therapies and personalized treatment strategies.
The Systemic Impact of Mitochondrial Dysfunction: A Multi-Organ Perspective
What is mitochondrial dysfunction, and how can it profoundly affect multiple organ systems, leading to a spectrum of complications? This question touches on a critical topic that many may not fully understand. In the nervous system, mitochondrial dysfunction is closely associated with neurodegenerative diseases such as Alzheimer's and Parkinson's, where oxidative stress plays a significant role in disease progression. This connection highlights the urgent need for further research into mitochondrial dysfunction and its potential as a primary event in energy production impairment related to these conditions.
The muscular system is not exempt from these challenges; cellular impairment can lead to myopathies, characterized by muscle weakness and fatigue. The heart, too, faces significant impacts, with conditions such as cardiomyopathy and arrhythmias emerging as potential complications. Understanding mitochondrial dysfunction is essential, as cellular impairment is linked to metabolic disorders like diabetes and has been associated with specific cancers, underscoring its systemic importance.
Recent discoveries reveal that over 96% of participants in studies related to cellular impairment reported medication use, indicating a high prevalence of treatment among affected individuals. This statistic emphasizes the importance of understanding cellular function for effective patient management and care.
Moreover, the systemic effects of cellular impairment extend to kidney issues linked to periodontitis, showcasing its extensive influence across various organ systems. As Zhengguo Cao, Chair and professor in the Department of Periodontology at Wuhan University, notes, "The interaction between cell energy failure and overall health is essential, especially in comprehending how it affects issues such as periodontitis."
As research continues to evolve, exploring therapeutic strategies, such as the combination of Proxison and Rapamycin for conditions like LAM disease, may open new avenues for addressing these complex interactions. This combination tackles various yet interconnected elements of cellular impairment, highlighting the necessity for innovative methods in therapy.
In summary, understanding the systemic implications of cellular impairment is crucial for comprehensive patient care. It impacts not only individual organ systems but also the overall health and well-being of patients. If you or someone you know is navigating these challenges, consider seeking support and resources that can provide guidance and understanding.
Recent Research and Future Directions in Mitochondrial Dysfunction
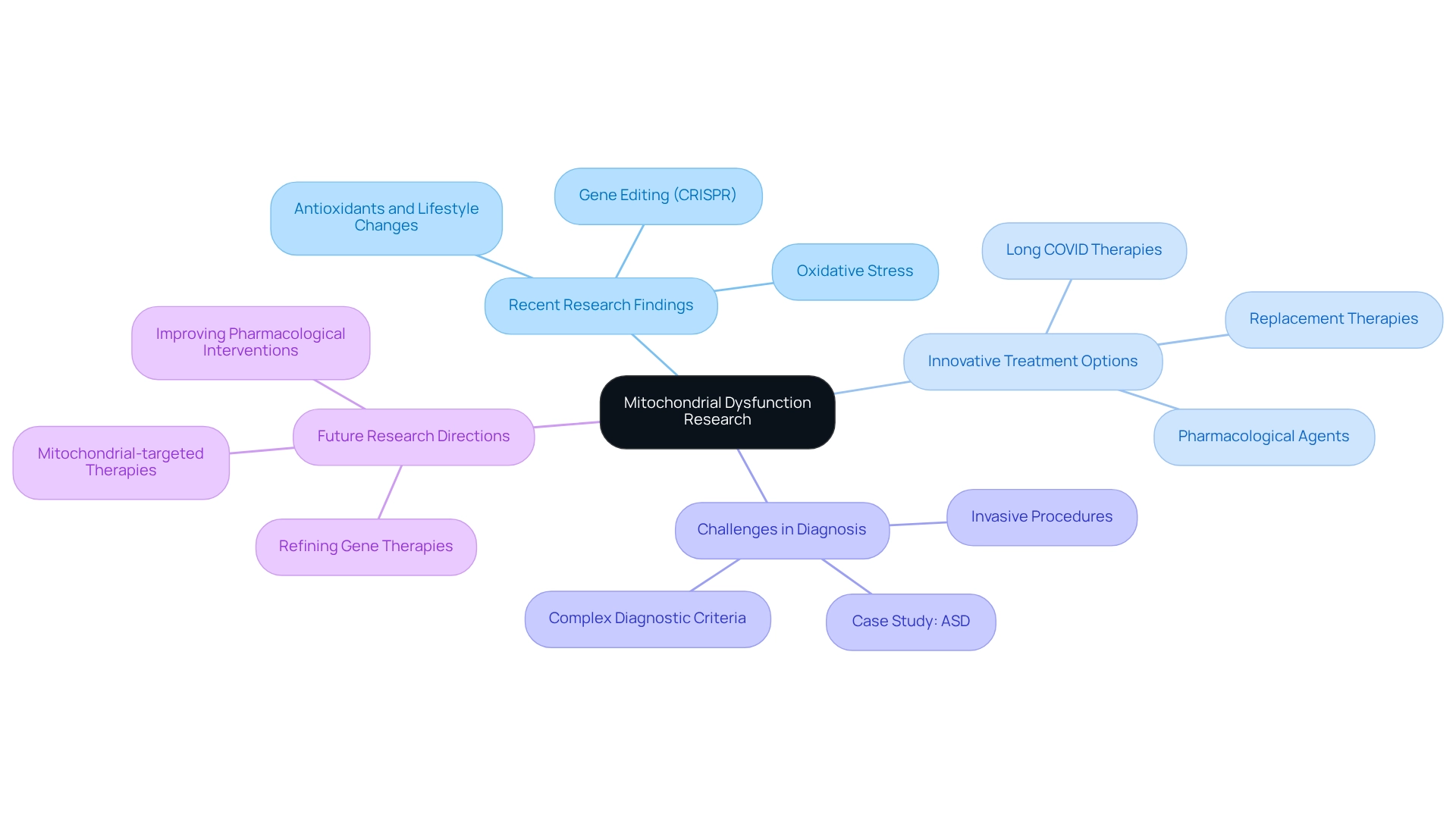
Recent research into cell power source dysfunction has made significant strides in uncovering the underlying mechanisms and identifying innovative treatment options that can bring hope to families. As we explore cellular processes, oxidative stress, and bioenergetics, we recognize their essential roles in various conditions that affect our loved ones. It’s alarming to note that every 30 minutes, a child is born who will develop a genetic disorder by age 10, underscoring the urgency of these studies and the need for support.
Understanding mitochondrial dysfunction is crucial, as it is a common factor in various viral infections and their long-term effects. This highlights the pressing need for continued research in this area, as we seek to protect our children’s health.
Advancements in gene editing technologies, particularly CRISPR, show promise for correcting mutations in cellular structures. This could potentially transform treatment paradigms, offering new avenues for hope. Furthermore, there is growing interest in replacement therapies and pharmacological agents aimed at improving cell function. For instance, recent clinical studies are investigating the effectiveness of antioxidants and lifestyle changes as therapies designed to enhance cellular energy production for conditions such as Long COVID. These efforts aim to restore cellular health and ease symptoms, which is a vital pursuit for families navigating these challenges.
Future research is essential to delve deeper into these therapies, providing the answers that many are seeking.
A recent case study titled 'Clinical Diagnosis of Mitochondrial Disease' sheds light on the complexities involved in diagnosing cellular disorders, especially in children with autism spectrum disorder (ASD). It emphasizes the necessity for comprehensive diagnostic criteria, including clinical signs and metabolic studies, while also acknowledging the challenges posed by invasive procedures like muscle biopsies. This complexity can be daunting for families, making it crucial to have clear pathways for diagnosis and support.
As research continues to evolve, translating these findings into clinical practice is vital for improving outcomes for individuals affected by mitochondrial dysfunction. Future directions in treatment will likely focus on refining gene therapies and developing more effective pharmacological interventions. This ongoing work paves the way for enhanced patient care and quality of life. As noted by Anne Rahbech, H.B.M., J.A.D., O.A., A.R., P.T.S., and C.D., the collaborative effort in advancing this critical field is a testament to our shared commitment to making a difference.
Conclusion
Mitochondrial dysfunction is a complex and multifaceted issue that touches the lives of millions, influencing various health conditions, from metabolic disorders to neurodegenerative diseases. The interplay of genetic mutations and environmental factors is crucial in the onset of these dysfunctions, emphasizing the need for a holistic approach to understanding and managing mitochondrial health. Advances in research, particularly genomic techniques and improved diagnostic methods, are opening doors for better detection and understanding of mitochondrial disorders. This progress is essential for timely intervention and effective treatment.
Recognizing the symptoms of mitochondrial dysfunction is vital for healthcare providers. Early diagnosis can significantly enhance patient outcomes, making it crucial to be vigilant. The diverse manifestations of these disorders call for a comprehensive and collaborative approach in clinical settings. This ensures that patients receive accurate diagnoses and tailored treatment plans that cater to their unique needs. Current treatment strategies focus on supportive care, dietary modifications, and emerging therapies, all aimed at improving the quality of life for those affected.
As research continues to evolve, staying informed about the latest developments in mitochondrial health is imperative. The systemic impact of mitochondrial dysfunction highlights the need for a broader understanding of how these organelles influence overall health and well-being. By fostering collaboration among researchers, healthcare professionals, and patient advocates, we can enhance the journey toward improved diagnosis, treatment, and advocacy for mitochondrial dysfunction. This collective effort holds the potential to transform the landscape of mitochondrial disease management, making it a pivotal area of focus for the future. Together, we can strive for better health outcomes for millions and support one another in this journey.
Frequently Asked Questions
What is the role of mitochondria in the cell?
Mitochondria are cellular organelles responsible for energy production, converting nutrients into adenosine triphosphate (ATP), which fuels cellular activities.
What are the consequences of mitochondrial dysfunction?
When mitochondrial function is compromised, it can lead to various medical challenges, including metabolic disorders and neurodegenerative conditions.
How prevalent is mitochondrial dysfunction in the USA?
Mitochondrial dysfunction affects over 50 million adults in the USA, who face diseases linked to primary or secondary dysfunction.
What advancements have been made in mitochondrial research?
Recent advancements, such as single-cell sequencing, have improved understanding of genomic diversity and mutations contributing to mitochondrial disorders.
How does single-cell sequencing contribute to mitochondrial illness research?
Single-cell sequencing allows for the examination of individual cells, revealing insights into phenotypic variability and tissue-specific expressions of defects in mitochondrial conditions.
Why is early recognition of mitochondrial dysfunction important in clinical settings?
Recognizing signs of energy impairment can lead to timely interventions and better wellness outcomes for affected individuals.
What factors contribute to mitochondrial dysfunction?
Mitochondrial dysfunction can arise from genetic mutations, environmental factors (such as exposure to toxins), and lifestyle factors (like poor nutrition and chronic stress).
How significant are genetic factors in mitochondrial dysfunction?
Genetic mutations, particularly those affecting mitochondrial DNA (mtDNA) or nuclear DNA, are significant contributors to mitochondrial dysfunction and may be inherited or spontaneous.
What role do environmental factors play in mitochondrial health?
Environmental factors, including exposure to toxins and certain medications, can severely disrupt cellular energy production, exacerbating mitochondrial dysfunction.
How can lifestyle choices impact mitochondrial function?
Poor nutrition, lack of physical activity, and chronic stress can worsen cellular dysfunction, highlighting the need for a holistic approach to health.
Why is genetic testing important for understanding mitochondrial disorders?
Genetic testing can identify mutations that contribute to mitochondrial dysfunction, aiding in the understanding of these conditions and supporting affected families.
What is the importance of patient registries and collaborative networks in mitochondrial research?
They provide valuable insights into the complexities of cellular energy disorders and foster a community of support for affected individuals and families.




